
What is Obstructive Sleep Apnea?
Obstructive Sleep Apnea (OSA) is a condition in which a patient’s muscles and tissues in the throat and air passage relax while sleeping, and this impedes the flow of air into the lungs due to a blockage of the airway. This can occur many times per night in the sleep cycle and especially during the REM sleep stages. Apnea is Greek for “without breath.”
Is Sleep Apnea Dangerous?
Here’s a list of the types of life-threatening conditions Sleep Apnea helps foster in a person affected by the disorder:
High Blood Pressure
Diabetes
Heart Disease
Stroke
It’s important to understand Sleep Apnea’s role in causing these issues. Sleep Apnea deprives a person of blood oxygen during the night, and as a result, the lack of oxygen puts extra strain on the heart. The extra strain on the heart can raise blood pressure and make it very difficult to control. High blood pressure can cause heart attack or stroke, and has its own set of complications.
If concerned about possibly danger of Sleep Apnea, it’s important to work with a care provider to help get it under control. When controlled, many of the cardiac symptoms can lessen and a person’s energy level and overall health can dramatically improve.
How Wellue Helps
Tracking and recording below vital signs at home regularly can help healthcare providers have a better understanding of your situations.

Blood Pressure
Wellue Blood pressure Monitor with EKG
For at-home instant and regular monitoring.
Can record long-term data for health insight.
Easily share the data with healthcare providers.

Diabetes Monitoring
Self-testing the blood sugar (blood glucose) can be an important tool in managing the diabetes and preventing complications. Wellue Checkme™ Suit enables at-home blood sugar testing every day.
More useful functions:
EKG Holter monitor for 24 hours.
ECG/EKG recorder
Infrared Thermometer
Tracking Oxygen Saturation
Sleep Apnea Screening
Tracking Blood Pressure
Touch Screen Operation

Preventing&Monitoring heart diease
Smart Heart Monitor
– Inexpensive way to help monitor heart rhythm at home.
– Great for monitoring Arrhythmia, heart failure, Atrial Fibrillation(Afib)…
– Responsive touch screen
– Easy to use and accurate
– Easily share ECG via phone or PC
Wellue Solutions for At-home Sleep Apnea Assessment
When a sleep apnea event happens, the blood oxygen level(pulse oximetry reading: SpO2) drops. Overnight blood oxygen level fluctuation can be used to assess sleep apnea or monitor the ongoing treatment.
Below are Wellue continuous oxygen monitors of different designs
– Tracking and recording overnight blood oxygen level fluctuation.
– Smart alarming function for abnormal blood oxygen or heart rate. It works by vibrating on your finger or wrist. This function can be turned off.
– Easily share the data with your healthcare provider.

O2Ring Continuous Ring Oxygen Monitor
Ring-shape design for comfortable sleep or daytime activity.
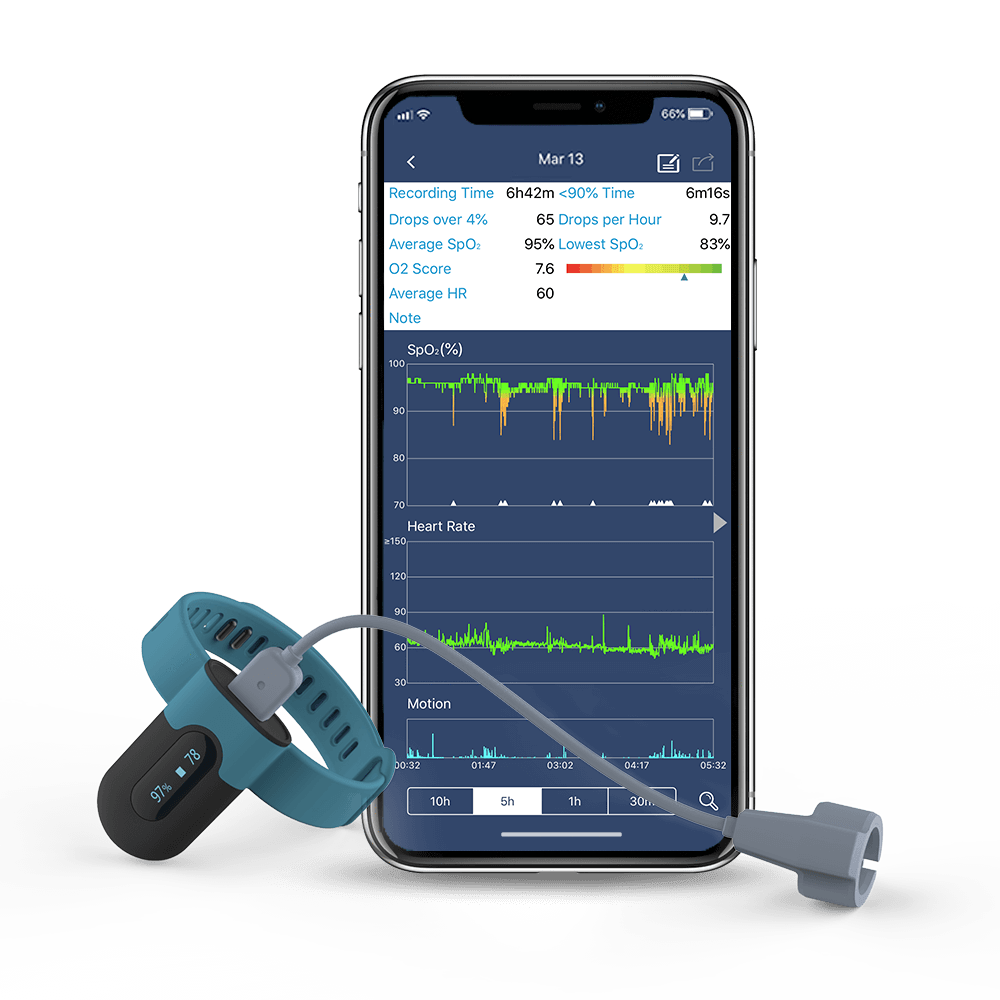
SleepU™ Wrist Oxygen Monitor
Wrist-style design.
Meet different tastes.

Checkme™ O2 Max Wrist Oxygen Monitor
With 72 hours extra-long battery life
I suspect I have sleep apnea, what should I do?
Sleep apnea is a serious and potentially fatal medical condition. If you or a loved one suspect you have it, you should see your doctor or be tested as soon as possible.
If your doctor suspects sleep apnea, they may recommend a sleep monitoring test. Also called a sleep study or polysomnography (PSG), it involves spending the night at a lab, clinic, or hospital. Your breathing and other vital signs will be monitored while you sleep.
It’s also possible to monitor your sleep in your own home. Your doctor might suggest at-home sleep monitoring if your symptoms and risk factors strongly suggest sleep apnea.
How often do I need to get supplies for my CPAP?
Regularly cleaning and replacing your mask, mask cushions, filters, and other CPAP equipment is vital in maintaining compliance. Various parts and pieces are scheduled to be replaced every so often as the materials in the equipment breakdown over time.
Most DME vendors will notify you when your equipment is due to be replaced. If you’re unsure of your replacement schedule or how often your insurance allows replacements, contact your DME provider and they will gladly check with your insurance company for you, so you don’t get any surprise bills in the mail.
Here is a general guideline for replacement parts:
Nasal interface – One every 3 months
Full face mask – One every 3 months
Nasal pillows – One per month
Nasal cushion – One per month
Full face cushion – one per month
Headgear – One every 6 months
Tubing – One every 3 months
Filter, disposable – Two per month
Filter, non-disposable – One every 6 months
Chinstrap – One every 6 months
Humidifier chamber – One every 6 months
If I lose weight, will I be able to get off CPAP therapy?
While weight and neck circumference are strong contributors to sleep apnea, they are not the only cause. Many people falsely believe that weight and neck size are the only causes of sleep apnea because they are the most obvious to point out.
Weight contributes to sleep apnea because of gravity and excessive tissues. When you sleep, the muscles of the body relax; this includes the muscles of the throat and mouth that work to keep your airway open during waking hours. People that are overweight often have larger necks and more soft fatty tissues in the throat. A narrower opening due to a thicker neck coupled with excess fatty tissue in the throat makes it easier for these tissues to fall back in the airway and restrict airflow.
However, many people that are not overweight also have sleep apnea for a variety of reasons. Some of these causes are:
Age – As people age their muscles begin to lose muscle tone. This is also true of the muscles in the throat. As throat muscles lose definition, they become weaker and more likely to collapse into the airways during sleep.
Enlarged tonsils or adenoids are the leading cause of obstructive sleep apnea in children but can also affect adults who never had a tonsillectomy when they were younger.
Natural causes – Some people can be genetically predisposed to having a narrower throat or may have an enlarged tongue that falls back into their airway. If your family has a history of OSA you are more likely to have it yourself.
Frequent alcohol use– Alcohol relaxes the muscles in the body, and this includes the throat muscles as well which may relax to the point of blocking the airway during sleep.
Smoking – Smoke is an irritant to the lungs, throat, and esophagus. It can cause inflammation and fluid retention in the upper airways that can impede airflow.
However, don’t let the idea of never getting off of CPAP discourage you from healthier lifestyle choices. While you may not be able to get off of CPAP entirely, losing weight can lead to less restrictive airflow, and therefore lower pressure settings, which can make therapy more tolerable.
Also, you may lose enough to put yourself in the mild to moderate group and qualify for a dental appliance as opposed to CPAP therapy.
