Article Overview
1. What is Asthma?
2. Symptoms of asthma
3. Diagnosis of Asthma
4. Understand Your Hypoxic Events Easily with Wellue O2ring
5. Estimated duration of Asthma
6. Prevention of Asthma
7. Treatment of Asthma
8. When to call a professional
What is Asthma?
Asthma is a chronic (long-term) lung disease. The airway narrows and becomes inflamed. This can cause breathing difficulties and wheeze.
Asthma ranges from mild to severe. Some people only experience mild symptoms occasionally. Others have almost constant severe, life-threatening symptoms.
During an asthma attack, the airways become inflamed. When the surrounding muscles contract, they narrow. The mucus produced by inflammation fills the narrow channels. As a result, the airflow is partially or completely blocked.
Asthma affects the larger and smaller airways of the lungs.
The cause of asthma-related inflammation is unclear. However, several environmental “triggers” have been identified.
Many causes of asthma are allergens. Allergens can cause some people’s immune system to overreact. Common allergens include:
- Animal dander and saliva
- Pollen
- Mould
- Dust mites
- Cockroaches
- Some medications
- Certain foods
Also ranked high on the list of asthma triggers are:
- Viral infections, such as colds and flu
- Exercise
- Breathe cold and dry air
Environmental pollutants, such as:
- Cigarette smoke
- Wood smoke
- Paint smell
- Chemicals
- Strong smell
- Emotional stress
For some people with severe asthma, no specific trigger can be determined.
Asthma can develop early, usually before 5 years of age. But its symptoms can start at any age. The condition has a genetic (genetic) component. It usually affects people with a family history of allergies.
Symptoms of Asthma
- Wheezing (whistle when air is forced out)
- Difficulty breathing
- Chest tightness
- Persistent cough
- For some patients with asthma, chronic cough is the main symptom.
Symptoms of a severe asthma attack may include:
- Extreme shortness of breath
- Chest tightness
- Fast pulse
- Sweating
- Dilated nostrils and pursed lips
- Need to sit upright
- Blue lips and nails
Between asthma attacks or sudden attacks, people with mild or moderate asthma may not have any symptoms.
In some people, symptoms only come on suddenly during or after exercise.
People with asthma who have an upper respiratory tract infection (such as a cold or flu) tend to have more severe symptoms.
Diagnosis of Asthma
Your doctor will ask:
- Do you have any symptoms
- How serious are they
- When and where they happened
- How often they occur
- What triggers and alleviates them
These details will help your doctor find ways to help prevent asthma attacks.
Your doctor will also want to know:
- Your personal history of allergies and respiratory diseases
- Your family history of asthma, allergies, and respiratory diseases
- Your doctor will listen to your back with a stethoscope to detect wheezing.
During the attack, your doctor can assess the severity of your sudden attack. He will listen to the airflow in your lungs. He will also observe how you use your chest muscles to breathe. Blue lips or skin indicate that you are not getting enough oxygen.
Other tests can be carried out in the office. These include measuring the speed of the air you can exhale forcefully. This is done by a device called a peak flow meter.
Another test called pulse oximetry measures the amount of oxygen in the blood. It is done by placing a small plastic clip on your fingertips.
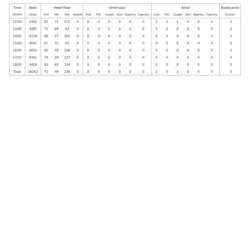
Understand Your Hypoxic Events Easily with Wellue O2ring
Wellue O2ring helps to track your blood oxygen level during your sleep, the report shows how long your oxygen is below 90%; how many times during a night your oxygen drops over 4%. You can also zoom into the chart to see more details, such as the exact value when dropping happens. You can easily share with your doctor for analyzing purposes.
During an asthma attack, blood tests may be done to check for infection. An arterial blood gas (ABG) test can be performed on blood samples. It provides more accurate oxygen level measurements. Your doctor may also want you to have a chest X-ray.
Two types of tests are commonly used to show how well your lungs are functioning:
Spirometry — This is a more thorough test. It is used to confirm the diagnosis of asthma. It also provides more detailed information about your lung function.
During spirometry, you exhale into a device that analyzes airflow and volume. After you take the bronchodilator, part of the test may be repeated. This medication relaxes the muscles around the airways. If you use bronchodilators to improve airflow, you have asthma.
Sometimes, when the spirometry shows normal, a provocation test is performed. For this test, you inhale the medicine to see if it causes your airway muscles to tighten. Asthma patients are more sensitive to this drug: their airway muscles are more likely to tighten.
Peak flow meter-this is a small portable tube. It can quickly and easily measure the airflow from the lungs. It measures the speed of the air expelled when you blow hard through it.
Peak flow meters are usually provided for asthma patients to use at home. They can use them to monitor their asthma. These devices help detect the earliest signs of an asthma attack.
Your doctor may want to do a blood test or allergy skin testing. These tests are used to determine specific substances (“allergens”) that can trigger an allergy.
Estimated duration of Asthma
Adult asthma is usually a lifelong disease. Through treatment, symptoms can be controlled. They may be uncommon or very mild.
In about half of children with asthma, asthma will go away on its own. Or it becomes less serious over time. However, it often reappears in later life.
Asthma attacks can go away on their own or with the help of asthma medications. The frequency and severity of attacks vary. It usually depends on the reason for triggering the attack.
Prevention of Asthma
Some asthma episodes can be prevented by avoiding or minimizing exposure to triggers.
These include environmental triggers such as:
- Cigarette smoke
- Environmental pollutants (especially when pollution and ozone levels are high)
- Strong chemicals
If exercise triggers your asthma:
- Breathe warm, humidified air before and during exercise
- Use inhalers before exercise
- Eliminating allergens at home often can go a long way to controlling asthma symptoms.
If dust mites are a trigger:
- Encase mattresses in airtight enclosures
- Clean your home frequently
- Wash bedding frequently in very hot water
- Remove carpets and heavy draperies from sleeping areas
Some people may need to avoid animals entirely. Others may benefit from taking preventive medicine before an anticipated exposure to animals. Pet owners should keep pets out of bedrooms and bathe them regularly.
Those who are affected by pollens should:
- Stay indoors whenever possible
- Use air conditioning
- Keep windows closed during the high pollen season
Prevention also means learning to anticipate future attacks. Monitor your symptoms and peak-flow readings to help identify a coming attack before symptoms develop. This allows you to adjust your medications to prevent an attack.
Early signs or symptoms of an asthma flare-up include:
- Coughing more often
- Increased mucus or phlegm
- Becoming short of breath quickly with exertion or exercise
- Developing a sinus headache or fever
Having symptoms that resemble a cold:
- Runny or congested nose
- Sneezing
- Watery eyes
Treatment of Asthma
The focus of treatment is:
- Prevent or stop inflammation
- Relax the muscles in the airway
If you have chronic asthma, please work with your doctor to develop an asthma management plan. The plan stipulates:
- How to avoid asthma triggers
- When and how to take medication regularly
- How to deal with acute attacks
- How to use a peak flow meter
There are several medicines that can be used to treat asthma. Some treat acute attacks (“rapid relievers”). Other prevent attacks from occurring (“controller”).
It is important to take preventive asthma medications as prescribed. You should take them even if you have no symptoms.
Bronchodilators. Bronchodilators relax the muscles around the airways to improve airflow. They are usually inhaled. One type of bronchodilator is called β-agonist. It includes salbutamol, metanephrine and pirbuterol. Beta-receptor agonists can be used alone as rapid relievers for mild and occasional symptoms. They are also used as “rescue” drugs to stop attacks. They can be inhaled with an inhaler or a nebulizer. A nebulizer is a device that mixes medicine with mist for inhalation. Other bronchodilators are used as “controllers” to reduce the number of asthma attacks. These include salmeterol (Serevent) and theophylline (several brands). They are not useful for asthma attacks because they take a long time to start working.
Anti-inflammatory drugs. These are controllers. Regardless of whether a person has asthma symptoms or not, they are usually taken regularly. They work by reducing inflammation. This reduces mucus production and reduces airway muscle contraction.
Anyone who has more than one asthma symptom every week should consider taking anti-inflammatory drugs. The first choice is usually inhaled corticosteroids.
When inhaled corticosteroids are not completely successful, corticosteroids can also be taken as pills. People who need urgent care or hospitalization usually get corticosteroids intravenously.
Other inhaled anti-inflammatory drugs can also be used. Leukotriene modulators are taken orally. These drugs block the chemicals that cause inflammation and narrow airways in many people with asthma.
Another anti-inflammatory drug is omalizumab (Xolair), which blocks inflammation by attacking IgE antibodies. IgE antibodies are the main participants in allergic reactions. This medication helps control the symptoms of severe allergic asthma patients who do not respond to other therapies and require frequent oral corticosteroids.
Immunotherapy. Some asthma patients also benefit from immunotherapy. In immunotherapy, patients will inject more and more allergens. The goal is to desensitize the human immune system. Immunotherapy seems to be most effective for mild to moderate asthma symptoms caused by sensitivity to indoor allergens.
Severe asthma attacks must be treated in a hospital. There, oxygen can be administered, and drugs may be given intravenously or with a nebulizer. In life-threatening cases, the patient may need a breathing tube placed in the large airway and artificial ventilation.
When to call a professional
Please call your doctor whenever you or your child continue to experience the following conditions:
- respite
- Chest tightness
- Difficulty breathing
- Cough
Some children with asthma may not particularly complain of shortness of breath. However, they may open their nostrils or use chest and neck muscles when breathing. These signs indicate that they are in trouble.
If you have been diagnosed with asthma, please call your doctor if you have the following symptoms:
- Getting worse
- Not controlled by conventional drugs
For example, if you must use emergency bronchodilators more than four times a day, call your doctor. Also, if your peak flow meter reading is in the yellow or red zone, please call.
If you have an asthma attack and your symptoms persist despite taking common medications, seek emergency help immediately.
Although asthma cannot be cured, it almost always can be controlled successfully. Most people with asthma lead relatively normal lives.